Paradigm Shift
Historically, device manufacturers for orthopedic and spine implants have focused largely on the surgeon as a primary customer. From the hospital’s perspective, the manufacturers lavishly catered to the physician while the hospital paid the bill, even as reimbursement declined. While some manufacturers still cling exclusively to this model, progressive device companies are starting to understand the limitations of traditional marketing and sales in favor of more holistic approaches to product development and sales. During this highly dynamic time there are opportunities to better understand and leverage knowledge of providers to more effectively serve customers.
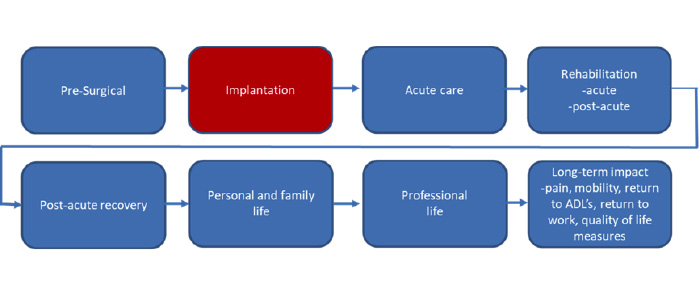
Although this article is written from the perspective of orthopedic, spine and neuroscience service lines, much of the content will have applicability across specialties. Healthcare “providers” can include hospitals, health systems, physicians, practices and other providers of healthcare services. Figure 1 illustrates the traditional model of selling to the physician and Purchasing at the time of implantation with minimal focus on the broader context of care and product lifecycle across the provider – patient continuum.
This article will provide insights on how Device/Diagnostics/Equipment/Technology (DDET) manufacturers can better understand their customers in a rapidly changing provider environment. My thesis is, by intimately understanding provider customers and their product use cycle, vendors can forge deeper relations that embed their products and themselves as preferred partners and ideally, not only selling to but, being pulled into strategic dialogue with executive administration/C-Suite.
Customers Are Changing; IDNs, Reimbursement, Supply Chain Processes
In the pursuit of scale and market share, hospitals, community-based services and practices have merged into multisite, multiservice organizational entities over larger geographies, oftentimes called Integrated Delivery Networks (IDNs). This has resulted in strategic reevaluation of service distribution within IDNs, and in some cases, the elimination or concentration of services at select locations. A manufacturer’s knowledge of this transforming provider environment is often limited beyond contact with typical touch points: Physicians, Purchasing and the supply chain. Understanding these developing realities can create strategic advantages for DDET.
The implications for vendors are several: increasingly centralized decision-making on purchasing, less influence among physicians due to more alignment with health systems, a heightened focus on demonstrable quality and the need to understand health systems beyond purchasing and the supply chain. Furthermore, in many of the reimbursement models already in place or being piloted, physician reimbursement will be impacted by selection of devices.
Although fee-for-service reimbursement is currently the dominant model, payment is inexorably moving to models such as bundling, total episode-of-care payment, capitation and other fixed-fee arrangements. This has required health systems to navigate new payment methodologies. While pay-for-performance can be financially rewarding, the learning curve is likely to increase the cost of business for providers and require fluency by DDET.
In the mid-term, providers will focus on reducing costs in both fee-for-service and value-based payment models by driving the management of the payment and accurately understanding and managing costs. Further, hospitals will focus and pursue DDET as first-line cost savings targets. Functional patient outcomes will become a core metric within provider systems, with implant/devices participating in comparative effectiveness studies making a contribution to understanding value.
What Do Hospitals/Health Systems Want Now?
In the constantly changing reimbursement environment, hospitals are scouring their organizations to reduce cost while improving quality. Current terms that describe these processes include: value analysis, low-cost/high value, process standardization, value-based reimbursement, and physician/hospital partnerships.
DDET alignment with these collaborative efforts in managing cost drivers can result in novel approaches and avoidance of commoditization of implants with the attendant downward price pressure. Moreover, newer reimbursement models and cost containment initiatives that impact physician reimbursement (bundled payment, gainsharing, co-management, and others) are challenging DDET brand loyalty and years-long relationships with manufacturers, potentially shifting preferences in favor of competitors that will bring greater value, lower price or patient benefit.
In the long term, more assertive initiatives such as population health will grow in prevalence with hospitals and physician specialists “packaging” services with an all-inclusive fee, with each provider applying a mindset of cost, value, outcome and service. As noted above, longitudinal data will be used to identify devices and procedures that produce favorable and differentiated outcomes.
Gathering Provider Intelligence
There are rich sources of provider information, insights and perspective into provider organizations that can inform DDET’s sales processes. In most cases this will requiring deliberate overtures to providers.
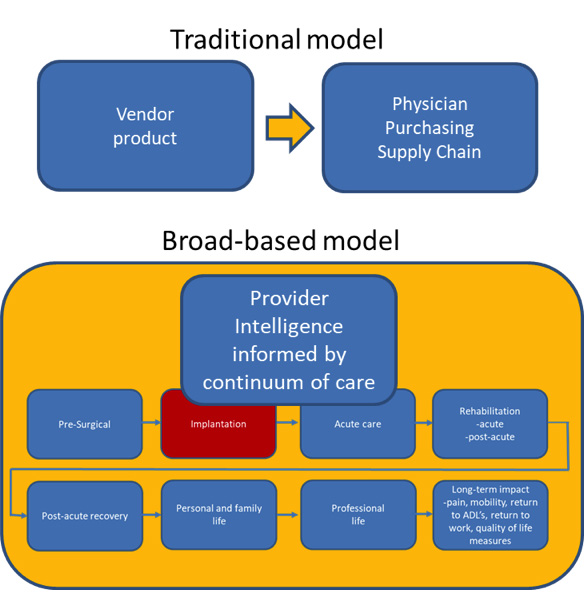
Vendors have the opportunity to collect and strategically apply insights from each customer. One approach, Provider Relational Modeling, is a process of collecting and applying a detailed understanding of vendor assets and provider business environments to identify key touch points across the organizations. The process envisions engaging with providers in a collaborative fashion that is characterized by fresh curiosity, an avoidance of presumption and receptivity to perspectives that may be foreign to the OEM/vendor. Areas of inquiry may include up to 20 or more provider departments and functions. The resulting vendor insights and capabilities represent strategic integration opportunities for vendors to design, develop and sell products that improve the quality of life for patients and create substantial value for providers clinically, functionally and financially. Figure 2 contrasts a traditional model of selling with a vendor and provider as stand-alone entities with a model that envisions the vendor as embedded and integrated with providers’ vision, goals and processes as illustrated in Figure 1.
Turning Insights into Action
Capitated, bundled and shared savings models associated with reform will reduce reimbursement and therefore place downward pressure on DDE pricing, in some cases with potential for disintermediation of distributors. DDETs will need to substantiate price with value and achieve reduced cost and/or improve quality. In looking at the emerging themes, they center on market access, with OEMs and vendors pursuing a more comprehensive understanding of their customers, fostering more effective provider-focused market research, furthering integration, collaborating and navigating their customer systems.
DDETs Opportunity and Mandate to Wear the Buyer’s Hat
As hospitals, health systems and their associated providers live in a more complex environment, traditional approaches to selling products and services have become less effective. Vendors who endeavor to both understand the customer environment, in its full continuum, and meaningfully invest in a partnership with providers can be rewarded with market share growth, reciprocal value and more permanence in their relations with providers and IDNs. To recap, OEM/vendors should aspire to:
- Deeply understanding hospital systems of care and how their product “lives” in the provider and patient environments
- Seek a seat at the “strategy table” with hospital leadership
- Offer demonstrably differentiated products with differentiated outcomes
- Achieve conversance in all reimbursement models: Fee for service, bundled payment, capitation, and risk
- Pursue collaborative, long-term relationships with IDNs and physicians